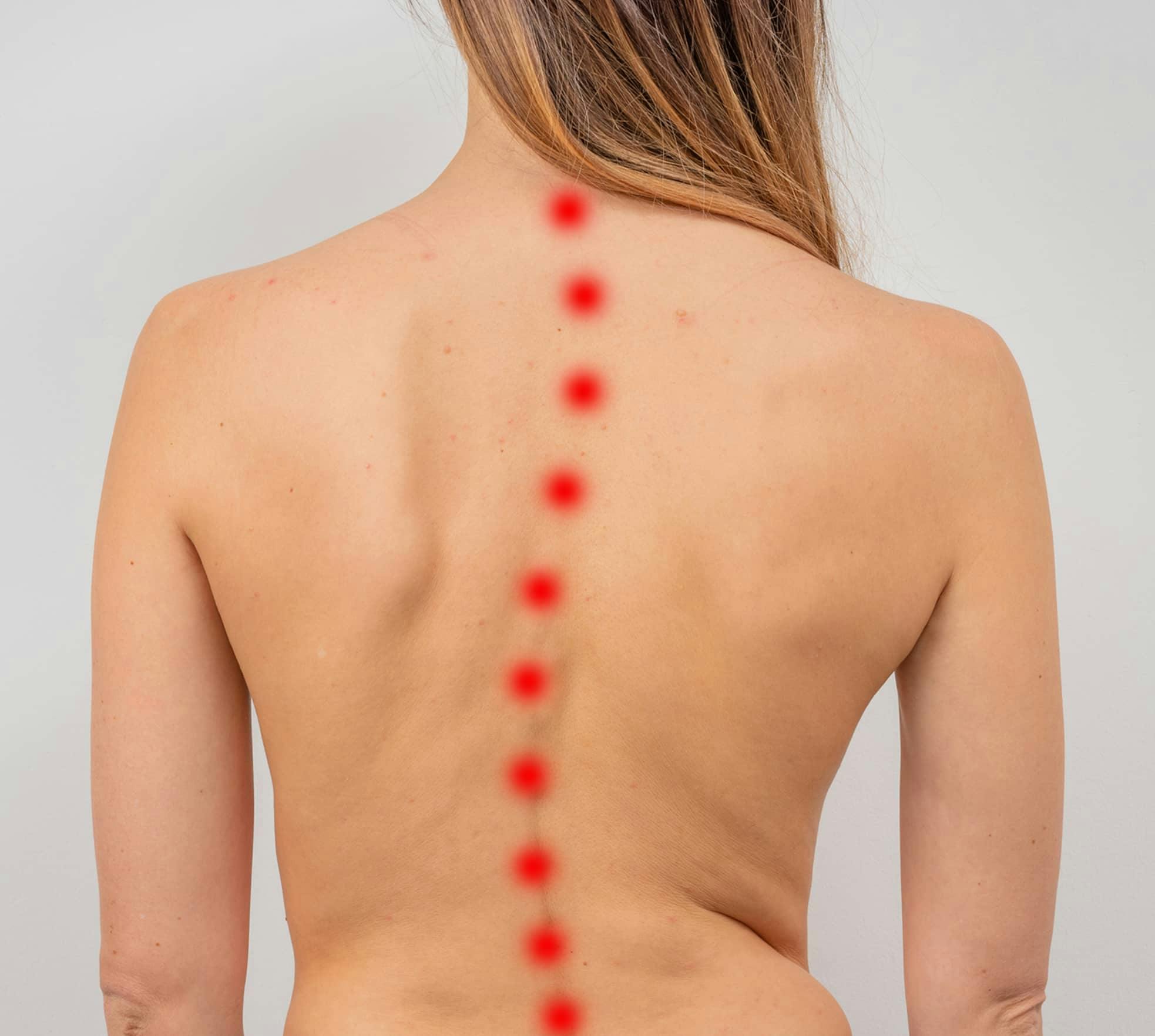
Scoliosis is a medical condition characterized by an abnormal curvature of the spine, often diagnosed during adolescence. The Center for the Functional Restoration of the Spine specializes in providing comprehensive care and innovative treatments to manage and correct scoliosis, aiming to improve patients' spinal health.
Scoliosis Q & A
What is scoliosis?
What type of scoliosis affects adults?
What symptoms develop due to scoliosis?
How do spine specialists treat scoliosis?
What is scoliosis?
Scoliosis occurs when your spine develops abnormal, side-to-side curves. When viewed from behind, your spine should form a straight line. If you have scoliosis, it creates a C- or S-shaped curve instead.
What type of scoliosis affects adults?
Most people think of scoliosis as a problem that begins in childhood or the early teen years, but the condition also appears in adults due to:
- Degenerative disc disease
- Facet joint arthritis
- Osteoporosis
- Congenital conditions
- Weak or paralyzed muscles
- Neuromuscular disease
The most common type of adult scoliosis, degenerative scoliosis, develops over the years. Problems such as arthritis and dehydrated discs gradually lead to an unstable spine and abnormal curves.
What symptoms develop due to scoliosis?
Degenerative scoliosis often causes a change in your appearance. The left and right side of your body may become uneven, with one shoulder or hip higher than the other. You may notice your body leans to one side or that your clothes don’t fit the way they should. Adults also develop mild to severe pain. The pain primarily arises from strained muscles, sprained ligaments, and stressed joints. You may also have compressed spinal nerves due to scoliosis. Pinched nerves cause pain, tingling, or numbness that travels down your arms or legs.
How do spine specialists treat scoliosis?
The team at the Center for the Functional Restoration of the Spine develops individualized treatment plans based on your symptoms and the severity of your scoliosis. Your treatment starts with conservative options such as physical therapy, bracing, and pain-relieving medications. Your provider also treats underlying conditions such as osteoporosis. If your pain persists, your provider at the Center for the Functional Restoration of the Spine may recommend interventional treatments, such as an epidural steroid injection or facet joint injection for long-lasting pain relief. As the last line of treatment, your provider may talk with you about surgery to correct the curvature or prevent the curve from getting worse. You may need procedures such as spinal fusion or spinal decompression. When performing a spinal fusion, the team may use robotic spine surgery to implant screws, rods, or other hardware. This advanced surgery uses 3D imaging and robotic-guided navigation to perform exact surgery. If you have back pain due to scoliosis, you can count on expert care at the Center for the Functional Restoration of the Spine. Call or schedule an appointment online today.