With a team of experienced spine specialists, the Center for the Functional Restoration of the Spine is dedicated to providing individualized care, helping patients regain mobility and improve their quality of life despite the challenges posed by sciatica.
Sciatica Q & A
What is sciatica?
What are the symptoms of sciatica?
Who is at risk of sciatica?
How is sciatica diagnosed?
How is sciatica treated?
What is sciatica?
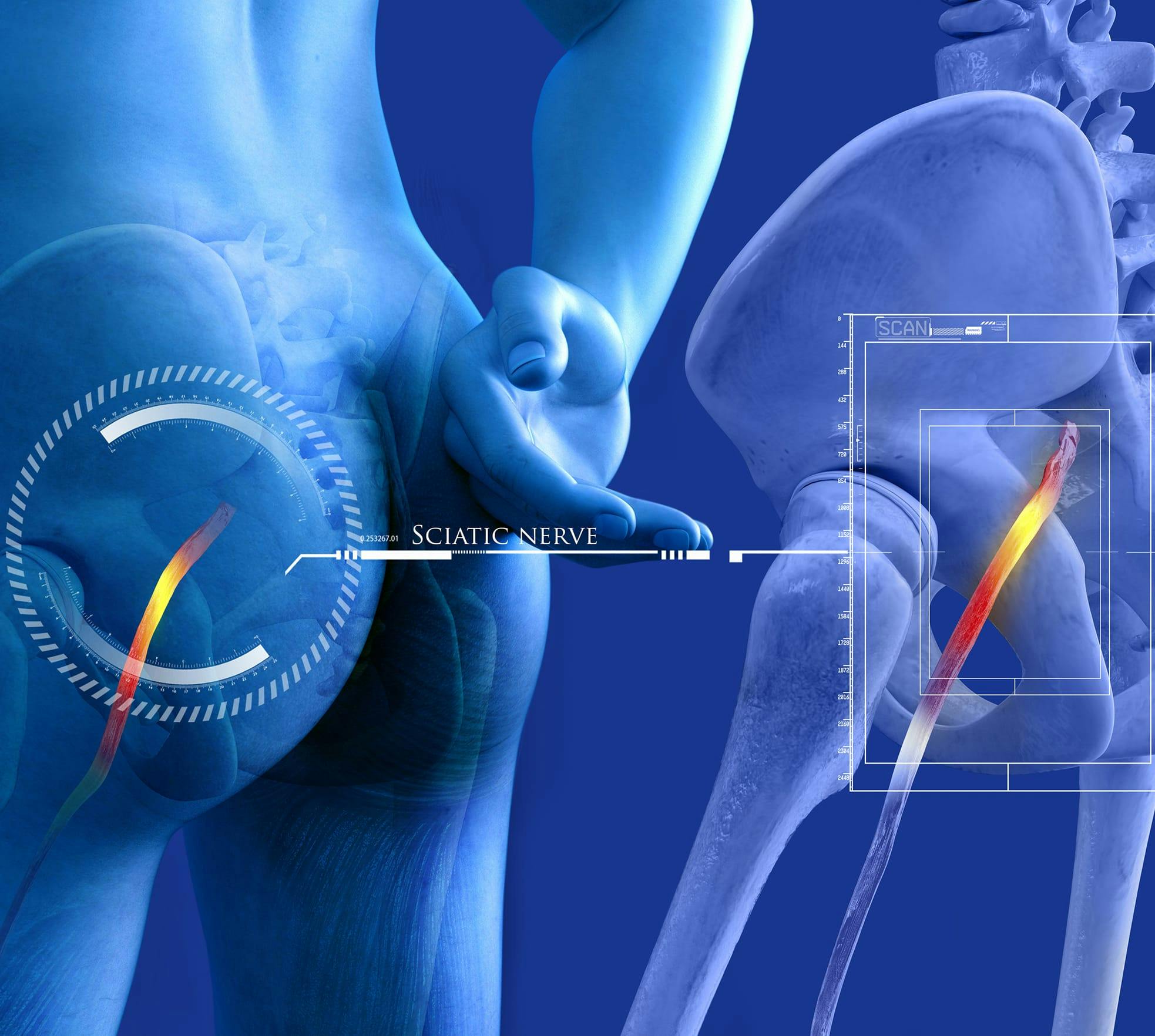
Sciatica is a painful condition that occurs as a result of undue pressure on your sciatic nerve. The sciatic nerve is the longest in your body and runs from your lower back to your buttocks and down your legs. Sciatica pain typically only affects one side of the body. The most common sciatica causes include auto injuries, herniated discs, bone spurs, and spinal stenosis.
What are the symptoms of sciatica?
The most common symptom of sciatica is lower back pain that radiates into your buttocks and legs. As it progresses, your leg pain may become worse than your back pain. You might also experience muscle weakness, tingling, or numbness in your feet, making it difficult to stand up, walk around, or exercise. Certain positions, such as standing or sitting, may aggravate your pain while lying down may provide the most relief. Pain caused by sciatica varies greatly. Some people only experience a dull ache while others suffer excruciating burning sensations.
Who is at risk of sciatica?
Sciatica affects people of all ages and backgrounds, but several factors may increase your risk, including:
- Being middle-aged or older
- Being overweight or obese
- Sitting for long periods
- Having diabetes
You are also more likely to experience sciatica if you have a physically demanding job. This is particularly true if you have to lift and carry objects or sit in one position for a long time.
How is sciatica diagnosed?
At the Center for the Functional Restoration of the Spine, your provider diagnoses sciatica by reviewing your medical history, asking about your symptoms, and conducting a physical exam. They also conduct a nerve root tension test, in which your doctor moves your legs in certain positions to stretch the sciatic nerve. If you feel pain during the test, it’s most likely you have sciatica.
How is sciatica treated?
The treatment for sciatica depends on the severity of your symptoms and their effect on your daily routine. Whenever possible, the Center for the Functional Restoration of the Spine recommends conservative, nonsurgical therapies, including:
- Medication
- Rest
- Physical therapy
If these treatments fail to provide relief or if nerve root compression is causing nerve damage, your doctor may recommend spine surgery to remove the pressure on the spinal nerve roots. Spinal decompression can be performed using a minimally invasive technique, allowing for a quicker recovery. Your surgeon discusses the risks and benefits of surgery with you to ensure you understand your options. To learn more about sciatica treatments, call the Center for the Functional Restoration of the Spine to schedule an appointment or book a consultation online today.