Trust the New Jersey Spine Specialists

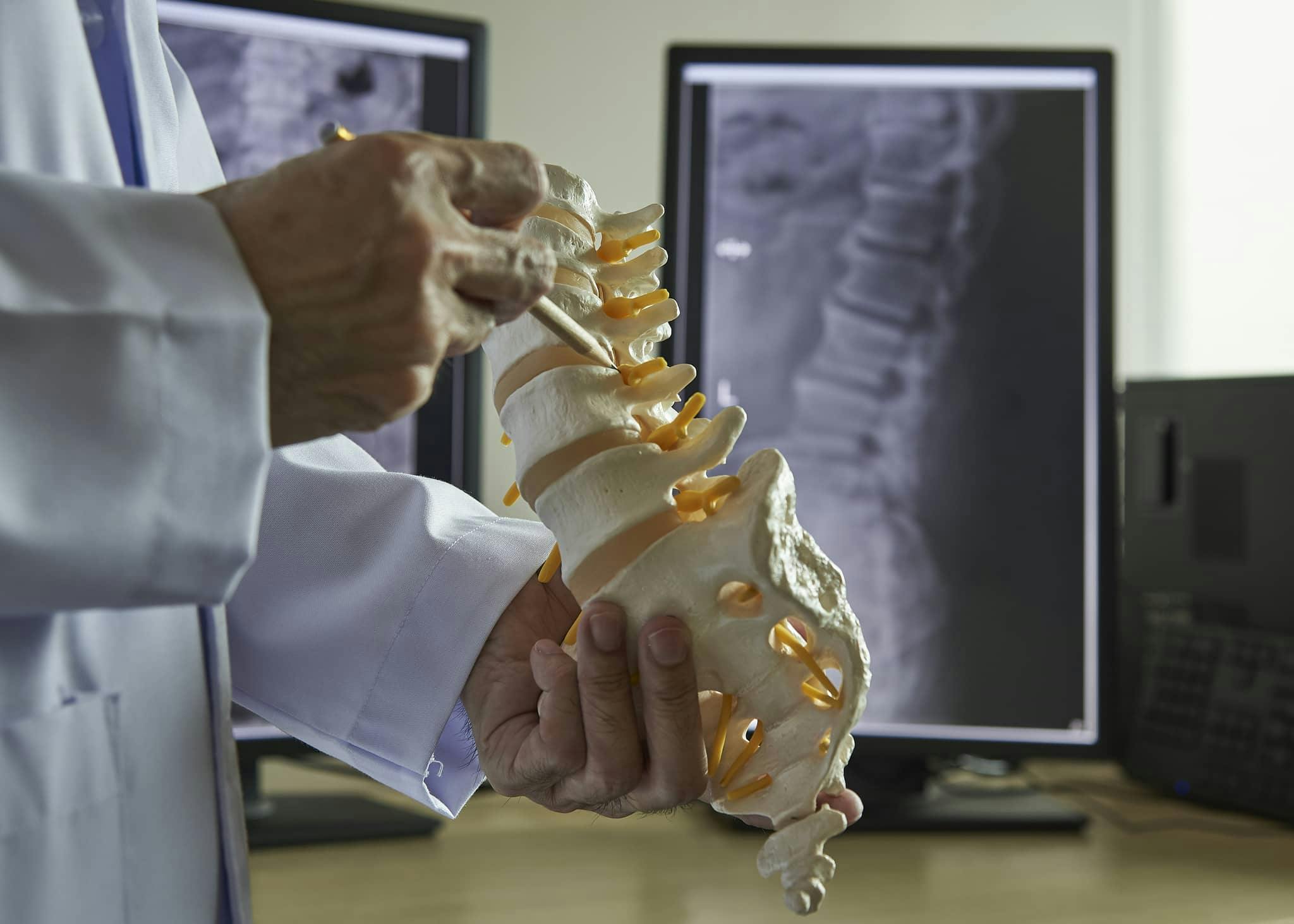
Minimally Invasive Solutions for Disc-Related Pain Relief
At the Center for the Functional Restoration of the Spine, we excel in providing minimally invasive orthopedic surgical solutions like Intradiscal Percutaneous Procedures to help you regain a pain-free and active life. Our entire orthopedic team is dedicated to providing cutting-edge treatments for various spinal conditions.
Disc Nucleoplasty
Disc nucleoplasty, or percutaneous disc nucleoplasty, is a minimally invasive procedure designed to alleviate the pain caused by herniated discs. This innovative treatment uses radio waves to vaporize small amounts of disc material, creating space within the disc.
As a result, the bulging disc material moves to fill the void, restoring the disc to its original shape. With the disc wall no longer herniated, pressure on nerve roots or the spinal cord is relieved, providing immediate pain relief.
Recovery from this outpatient procedure is typically swift, as it doesn't require muscle or bone cutting. With limited bed rest and a tailored physical therapy program, patients often return to their normal activities within one to six weeks.

IDET (Introdiscal Electro Thermal Therapy)
IDET, or intradiscal electrothermal therapy, is a minimally invasive outpatient procedure designed to alleviate chronic or severe low-back pain stemming from diseased, damaged, herniated, or degenerated discs. During IDET, an electrothermal catheter equipped with a thin heating wire is used to deliver precise amounts of heat to the affected disc. This process helps seal cracks in the disc's outer wall, reduce herniated disc bulges, and cauterize and disable painful nerve endings affected by the deformed disc.
Degenerative disc conditions, often related to aging, can lead to cracks in the intervertebral disc wall or herniated discs, causing debilitating lower back pain. IDET leverages heat to repair some of these effects, significantly reducing pain in many patients. Although some discomfort may occur during the procedure, it indicates that your physician has located the source of pain accurately. IDET provides relief or elimination of chronic lower back pain and improved mobility in approximately 80% of patients.
Dekompressor Discectomy
A discectomy involves the removal of a portion of a herniated disc that irritates a nerve, causing pain. In the minimally invasive dekompressor discectomy, a small needle is guided to the herniated disc using an advanced X-ray technique called fluoroscopy. A probe with a rotating tip is then inserted through the needle to reach the herniated disc. When activated, the probe's tip drills away part of the disc nucleus, creating space for the herniated disc wall and relieving pressure on the nerve. The dekompressor discectomy is a commonly performed procedure aimed at preserving or restoring neurological function, stabilizing spinal segments, improving functionality, and relieving pain. Typically, this operation is performed on patients experiencing back and leg pain for at least six weeks, often due to excessive pressure on a nerve. The procedure can be performed using open surgery, typically requiring a 1-1/2 inch incision, depending on the location and severity of disc damage.


It’s Time to Choose a Pain-Free Life
At the Center for the Functional Restoration of the Spine in Edison, Shrewsbury, and Toms River, NJ, we have particular expertise in Intradiscal Percutaneous Procedures and other advanced techniques. Our patient-centered approach ensures you receive personalized care and faster recovery times with effective pain relief. Contact us today to start your journey.

